I’ll help you create a blog post on “How To Diagnose Celiac Disease” following the specified guidelines. I’ll first use a web search to gather accurate, up-to-date information. Based on the search results, I’ll craft the blog post following the specified guidelines:
Celiac disease is a complex autoimmune condition that affects approximately 1% of the population, yet remains significantly underdiagnosed. With an estimated 80% of cases undetected or diagnosed after years of suffering, understanding how to diagnose this condition has become increasingly critical. Recent advances in medical diagnostics have transformed our approach to identifying celiac disease, offering hope to those struggling with unexplained symptoms.
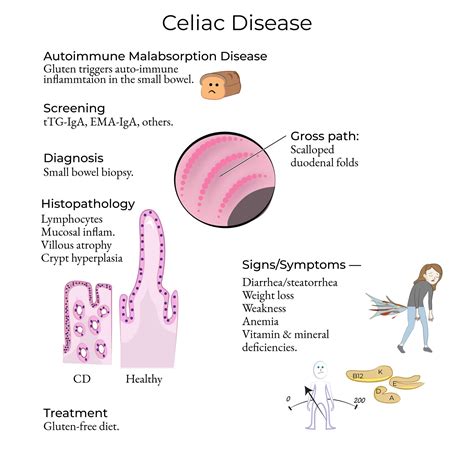
Understanding Celiac Disease Diagnosis

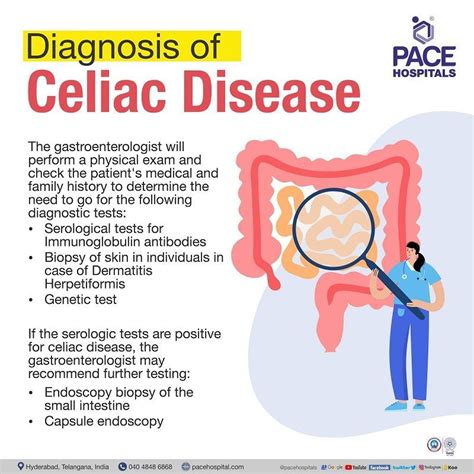
Diagnosing celiac disease is a systematic, multi-step process that requires careful medical evaluation. The diagnostic journey involves several key components designed to provide accurate and comprehensive assessment:
Clinical Assessment and Symptom Evaluation

Celiac disease presents with a wide range of symptoms that can often be mistaken for other conditions. Common indicators include:
- Chronic digestive problems
- Unexplained fatigue
- Persistent anemia
- Skin rashes
- Neurological issues
- Unexplained weight loss
- Chronic diarrhea or constipation
Serological Testing: The First Diagnostic Step

Blood tests play a crucial role in celiac disease diagnosis. The primary screening method involves:
- Tissue Transglutaminase IgA (tTG-IgA) Test: This is the most sensitive initial screening, with 93% accuracy for patients on a gluten-containing diet.
- Total IgA Antibody Test: Ensures the patient produces sufficient antibodies for accurate testing.
- Deamidated Gliadin Peptide (DGP) Antibodies: Particularly useful for young children and complex cases.
Genetic Testing Considerations

While genetic testing cannot definitively diagnose celiac disease, it provides valuable insights:
- HLA-DQ2 and HLA-DQ8 Gene Screening: Can help rule out celiac disease if these genes are absent.
- Useful for Family Screening: First-degree relatives have a 1 in 10 risk compared to 1 in 100 in the general population.
Intestinal Biopsy: Confirmatory Procedure

Traditionally, an upper endoscopy with small intestine biopsy has been the gold standard for diagnosis. Recent 2025 guidelines from the European Society for the Study of Coeliac Disease have introduced more flexible approaches:
- For symptomatic adults under 45 with extremely high antibody levels
- Potential diagnosis based on blood work alone in carefully defined situations
- 98-99% accuracy when antibody levels are significantly elevated
🩺 Note: Always maintain a gluten-containing diet during testing to ensure accurate results. Premature elimination of gluten can complicate diagnosis.
Special Diagnostic Considerations

Pediatric Diagnosis
- Screening typically begins around ages 2-3
- Requires special antibody panels
- Genetic testing can provide early insights
Seronegative Cases
Approximately 5-10% of patients may have negative serology despite active disease, requiring more comprehensive evaluation.
Emerging Diagnostic Innovations
As of 2026, exciting developments are transforming celiac disease diagnosis:
- IL-2 Blood Test: Currently in clinical trials
- Potential to eliminate traditional gluten challenge
- Expected availability in 2026-2027
Key Takeaways for Potential Patients

- Do not self-diagnose
- Maintain gluten intake during testing
- Consult a gastroenterology specialist
- Consider family history and genetic risk
The landscape of celiac disease diagnosis continues to evolve, offering more precise, patient-friendly approaches to identifying this complex autoimmune condition.
How long does the diagnostic process take?
+
The diagnostic process typically takes several weeks to a few months, involving multiple tests and potential specialist consultations.
Can I be diagnosed if I’m already gluten-free?

+
You may need to undergo a gluten challenge, consuming gluten for 6-8 weeks before testing. Always consult with a healthcare professional to determine the best approach.
Are there risks of misdiagnosis?

+
Yes, symptoms of celiac disease can mimic other conditions like IBS or inflammatory bowel disease. Professional medical evaluation is crucial for accurate diagnosis.